Author: Ken Hoffman
Peer reviewers: Chris Nickson, Arne Diehl
Everything ECMO 015
The emergency alarm goes off in the ICU and you are the first doctor to arrive.
The patient is a 45-year-old man transferred to the unit and started on extracorporeal membrane oxygenation (ECMO) two hours prior.
Q1. What is the first thing you should determine if a patient arrests on ECMO?
The first thing to establish is whether the patient is on VA or VV ECMO.
- VV ECMO – Cardiac arrest is associated with a complete loss of cardiac output as the native heart is acting as the pump
- VA ECMO – The ECMO circuit likely provides at least partial circulatory support despite the arrhythmia as the ECMO machine is acting as the pump
Q2. You establish that the patient is on VA ECMO and has had a cardiac arrest, what should you check next?
The next thing to check is the ECMO circuit flow and the blood pressure.
If the circuit flow is able to maintain systemic perfusion (e.g. >4L/min) then you have time to think!
If the circuit is not flowing, assess urgently for circuit factors:
- Pump failure – the ECMO machine will have stopped, clamp the circuit, transfer to the emergency drive unit (the “hand crank”). Check the power supply; you may need to exchange the ECMO unit.
- Decannulation or circuit rupture – this will be self evident and messy, clamp the circuit and turn off the pump to prevent further air embolism or exsanguination, apply pressure to any bleeding sites, then manage the patient as per ALS – emergent recannulation.
- Air embolism – clamp the circuit on the return line and turn off the pump, position the patient head down and manage as per ALS, consider aspirating the right atrium and/or right ventricle.
- Fulminant circuit or pump head thrombosis, clamp the circuit and manage the patient.
Q3. Should you do chest compressions for cardiac arrest in a patient on VA ECMO?
This depends on whether the ECMO circuit is still perfusing the patient.
- If the circuit is maintaining systemic perfusion then you do NOT need to perform chest compressions. Even brief periods of low flow can usually be tolerated.
- If there is pump failure, switch to the hand crank immediately.
- If there is no circuit flow (see above), then you should manage as per ALS guidelines until ECMO flow is re-established. Adrenaline boluses in the 1-2 minutes before re-initiating ECMO support should be avoided.
Q4. What will the arterial line show in a VA ECMO arrest?
There will be a loss of arterial pulsatility due to a loss of native cardiac output.
This will result in an arterial “flat line” trace and the mean arterial pressure (MAP) will likely drop depending on amount of ECMO support and the patient’s total peripheral resistance.
Q5. What rhythms would you expect to see?
The rhythm may be a non-shockable or shockable rhythm.
- Non-shockable rhythms are asystole and pulseless electrical activity (PEA).
- Shockable rhythms are ventricular fibrillation (VF) and ventricular tachycardia (VT).

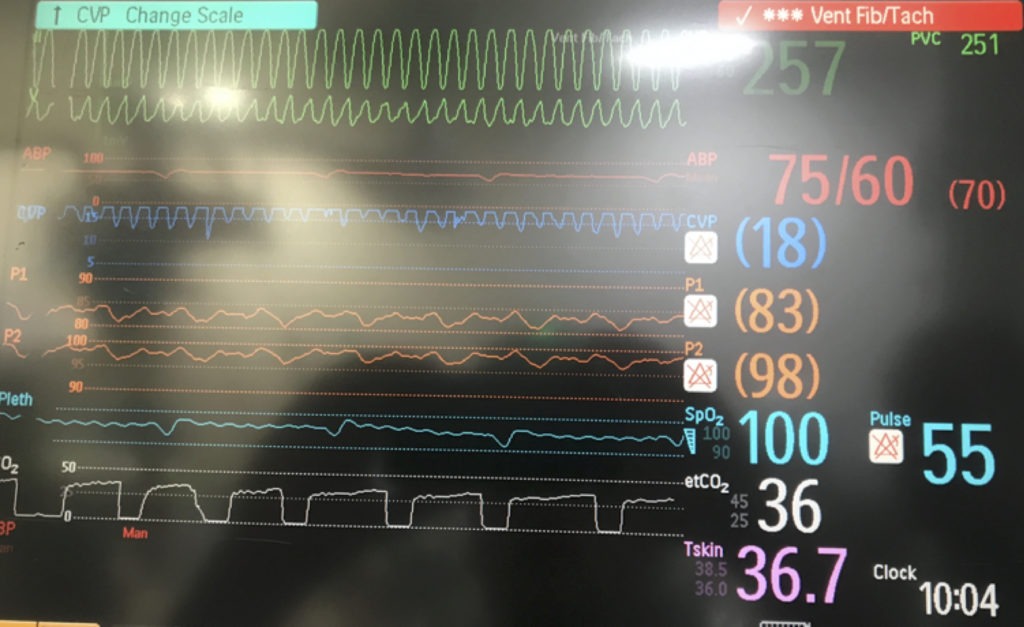
Monitor showing ventricular fibrillation in a patient supported by VA ECMO.
Side note: Is a PEA arrest on ECMO a “thing”?
- These are patients with loss of native cardiac output or various degrees of cardiogenic shock. The term PEA whilst technically correct is generally not used in these circumstances ,instead we talk about loss of pulsatility secondary to poor native cardiac output or poor aortic valve opening that results in an undetectable pulse.
- If the patient has severe cardiogenic shock they may not have a palpable pulse or even visible pulsatility on their arterial line trace. Whilst this would technically fit the definition of PEA, an echo may actually show some cardiac movement. In this setting loss of pulsatility reflects severe heart failure rather than an arrest. Increasingly the term “pseudo-PEA” is being used for cases such as this, where true “electro-mechanical dissociation” is absent.
Q6. What are the treatment priorities in a cardiac arrest in a VA ECMO patient?
There is no universally standardised approach for these patients with mechanically supported circulation. In particular adrenaline IV boluses are NOT indicated. Ensure that support with VA ECMO is adequate.
The following principles apply whilst trying to identify and correct the underlying cause:
Shockable VT/VF
- Defibrillation — 150J
- some experts use an initial 100J for VT on VA ECMO
- consider delaying subsequent shocks until after correction of reversible factors and loading with anti-arrhythmics if refractory
- Amiodarone 300mg IV after the third shock
- Avoid 1mg adrenaline boluses, consider titrating vasopressors to target MAP
Non-shockable Asystole/PEA
- Avoid 1mg adrenaline boluses, consider titrating inopressors to target MAP
Some other things to remember when managing cardiac arrest on VA ECMO:
- Get help! Ensure the ICU Consultant and ECLS Coordinator are notified ASAP.
- Decrease lung ventilation (pulmonary blood flow is usually minimal). Required respiratory rate may typically be 2-4 breaths per minute during cardiac arrest on VA ECMO.
- After reversion, ventilator, ECMO blood flow settings, and inotrope and vasopressor support will need to be adjusted
Note that it is possible for a patient receiving VA ECMO to be awake, at least to some degree, during a cardiac arrest… which can have important management implications! Always consider the need for explanation and the need for analgesia and sedation before administering uncomfortable therapeutic interventions.
Q7. What can cause an arrest on VA ECMO?
Important causes grouped according to the traditional ALS ‘Hs and Ts’:
- Hypoxia
- turn both the ventilator and ECMO oxygen blender to FiO2 to 1.0
- ensure O2 is flowing to the oxygenator
- check for colour change across the oxygenator (bright red blood in the return line)
- check a pre-oxygenator and post-oxygenator blood gas if required
- Hyperkalaemia
- check K+ on arterial blood gas and consider haemolysis
- Hypovolaemia
- consider giving fluid bolus
- check Hb
- consider retroperitoneal bleeding from cannula insertion
- Hypothermia
- check body temperature and ECMO heater unit function
- cooling occurs rapidly if the ECMO heater unit is not functioning (e.g. ECMO initiation, during transfer)
- Tamponade
- focused transthoracic echocardiography (TTE) initially, transoesophageal echocardiography (TOE) TOE if indeterminate and patient is sufficiently stable.
- If present, or other causes excluded, contact Cardiothoracics and prepare for sternotomy
- tamponade physiology is complex in VA ECMO, but can cause access insufficiency
- Tension pneumothorax
- uncommon in VA ECMO
- consider especially if difficult to ventilate; focused thoracic ultrasound may help confirm pleural sliding
- may occur if an intercostal catheter is blocked or displaced
- Thrombus
- consider ongoing or new myocardial ischaemia, or pulmonary embolism
- Toxins
- check history to see if toxins were the cause of going on VA ECMO (e.g. calcium channel blocker overdose) as specific antidotal management may be required
- loss of pulsatility can occur with even relatively low doses of beta blockers or sedatives in patients with cardiogenic shock on VA ECMO
Also consider:
- progression of the underlying disease state (e.g. fulminant myocarditis causing progressive cardiogenic shock or arrhythmias)
- a problem with the arterial line mimicking PEA (always check the pulse the old-fashioned way!)
Q8. What complication may occur with loss of native cardiac output, even if the patient is fully supported on VA ECMO?
A lack of forward blood flow through the left ventricle has resulted in stasis of blood in the left ventricle.
Thrombosis occurs when forward blood flow and aortic opening is not restored in a timely fashion. This complication is usually catastrophic.
Prolonged impaired pulsatility can also lead to progressive left ventricular distention and potential for aortic regurgitation, which can cause acute pulmonary oedema and render VA ECMO support ineffective.
Key References
- Nickson CP. Pulseless Electrical Activity (PEA). Critical Care Compendium, Lifeinthefastlane.com. 6 September 2015. [Accessed: 1 November 2017]. Available at URL: https://lifeinthefastlane.com/ccc/pulseless-electrical-activity-pea/
- Pellegrino V, Sheldrake J, Murphy D, Hockings L, Roberts L. Extracorporeal Membrane Oxygenation (ECMO). Alfred ICU Guideline, 2012.

Fantastic narration.
Good thank you for much information.
One question i’ll give.
There go two sentences about adrenaline bolus.
Q3 (Should you do chest compressions for cardiac arrest in a patient on VA ECMO?): “If there is no circuit flow (see above), then you should manage as per ALS guidelines until ECMO flow is re-established. Adrenaline boluses in the minutes before ECMO support should be avoided”
Q6. What are the treatment priorities in a cardiac arrest in a VA ECMO patient?
Non-shockable Asystole/PEA: “Avoid 1mg adrenaline boluses, consider titrating inopressors to target MAP”
What is the reason for avoiding epinephrine bolus? To where Is this harm?
For stimulating heart rhythm, i think epinephrine bolus is necessary at cardiac arrest.
And this is opposite to “Alfred ICU Guideline, 2012” which you gave me as a reference.
Please let me know. I’ll appreciate it. =)
Hi
Cardiac Arrest in a patient already on VA ECMO:
If a patient has a cardiac arrest on ECMO, they typically already have an arterial line in and often we will titrate a norepinephrine infusion to achieve a target BP (e.g. if PEA). If a shockable rhythm, the priority is defibrillation and usually BP can often be maintained without adrenaline boluses. In a patient on support MAP is usually reasonably well maintained, they may need additional vasopressor support, but large boluses of adrenaline will likely cause a hypertensive surge.
In ECPR, or no longer on VA ECMO support (e.g. pump failure):
We typically give adrenaline/ epinephrine 1mg IV boluses as per ACLS protocol during cardiac arrest.
In an ECPR, in the two minutes or so prior to going “on pump” we typically avoid giving further adrenaline doses to avoid a hypertensive surge.
Alternate strategies (which have rationales, but lack a strong evidence base) include:
– Some centers (e.g. in France) limit the does of adrenaline given during cardiac arrest to 5mg IV total.
– Others, if an arterial line is available, will run an epi/norepinephrine infusion and titrate it to DBP to maintain coronary perfusion.
These are situations – either refractory arrest where standard ALS has failed, or a pateint on ECMO support – where standard ALS guidance does not apply.
Cheers
Chris
Hi,
Thank you for the great summary. For Q 6., if a patient presents with persistent VT/VF right after E-CPR, should defibrillation be continued before transferring the patient to a cath lab? There is very limited literature on this issue. I understand that my question is in a different context to your summary. Could you kindly share the reference of your answer on question 6 that defibrillation should still be delivered on a patient with an ECMO.
Thank you!
It is quite common for patients in VT/VF resistant to defibrillation to be successfully defibrillated after a few minutes of VA-ECMO perfusion.
It is worth trying once the patient is on pump.