Author: Lynda Thurston
Reviewers: Chris Nickson, Aidan Burrell
Everything ECMO 006
A 40 year-old man with necrotizing pneumonia is receiving V-V ECMO support. He has been converted to a high-flow configuration (access cannulae in the right internal jugular vein in addition to the right femoral vein) to manage persistent access insufficiency.
Unfortunately, despite this, he continues to have access problems.
This is his CXR:
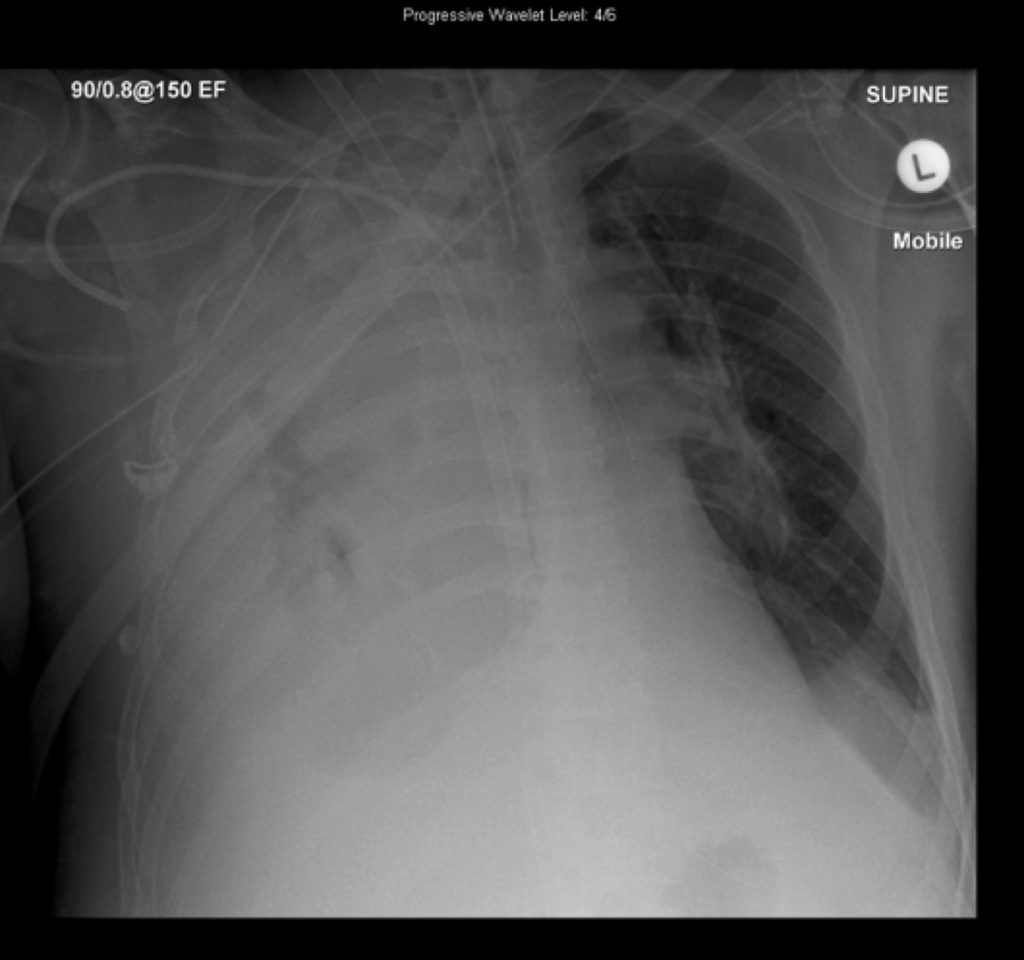
Q1. What problems may be contributing to persistent access insufficiency in this scenario?
The important differentials include:
- Hypovolaemia due to haemorrhage / haemothorax
- Compression of the superior vena cava and/or the right atrium from haemothorax or massive pleural effusion (“tamponade effect”)
- Complications from ECMO cannula insertion in the neck (e.g. local haematoma)
- Thrombosis at the access cannula (less likely to be a factor given the recent change to a high flow VV-ECMO configuration)
- Kinking or obstruction of the circuit
Echocardiography with lung ultrasound is performed at the bedside. This confirms the presence of large loculated pleural effusion is compressing his superior vena cava (SVC) and right atrium (RA).
Q2. What are the management options?
Potential therapies include:
- Conservative / supportive management (as described in Everything ECMO 003: reduce ECMO flows to prevent “suckdown”, continue to optimize preload and vasoconstriction, prevent changes in intrathoracic pressure with adequate sedation and paralysis)
- Intercostal catheter insertion (but drainage is unlikely to resolve loculated collection)
- Video-assisted thoracoscopic surgery (VATS)
Q3. What are the risks of surgical intervention while the patient is receiving ECMO support?
The risk of bleeding with any procedure performed on an ECMO patient is significant and potentially life threatening. Haemorrhage is the most common complication of ECMO, due to the need to anticoagulate the circuit as well as circuit related factors.
All interventions require a careful weighing of the risks and benefits.
You manage to provide support for him for two more days despite the access insufficiency (Sa02 > 90%, HR <120/min, noradrenaline <10 mcg/min, lactate <4 mmol/L) but eventually decide, following discussion with your cardiothoracic surgical team, to proceed with a VATS procedure.
Q4. How will you manage the patient’s anticoagulation?
Most ECMO centers advocate withholding anticoagulation for 12 hours prior to, and 24 hours after, major procedures.
Modern ECMO circuits are entirely heparin-bonded, which decreases the risk of circuit thrombosis over short periods in the absence of systemic anticoagulation compared to older circuits.
On return from the operating theatre following the VATS procedure, the patient remains stable.
Ten hours later, a routine plasma-free haemoglobin (PFHb) measurement comes back at 0.11 g/dL.
Q5. What does this laboratory result suggest?
A PFHb > 0.10 g/dL is a sensitive indicator of haemolysis. In a non-anticoagulated ECMO patient this raises the concern that circuit thrombosis is starting to occur, which can cause haemolysis.
Artefactually elevated PFHb levels can result from sub-optimal blood collection. If there is a low index of suspicion for haemolysis, a repeat sample should be checked.
In this case, the elevated PFHb level is confirmed. Given this information, you decide to restart a heparin infusion.
Five hours after restarting IV heparin, the patient becomes hypotensive with escalating noradrenaline requirements. You notice that 1L of blood has “dumped” out of his right-sided chest drain.
Q6. What is your approach to the management of this new issue?
Significant haemorrhage from a necrotic lung can be very difficult to control. This patient has a high risk of death.
Management involves:
Resuscitation
- Stop heparin and consider reversal with protamine (though this risks circuit thrombosis, it may be essential in life-threatening haemorrhage)
- Activate the massive transfusion protocol
- use a blood warmer for rapid fluid administration via large bore access (e.g. swan sheath or RICC line) with early use of blood products
- consult the on call transfusion haematologist
- Assess clotting profile, and correct coagulopathy and other bleeding diatheses if present (e.g. platelets, INR, hypocalcaemia, and potentially reversible pro-haemorrhagic medications)
- Correct acidosis and avoid hypothermia
Consider further surgical intervention
- Urgently consult with the cardiothoracic surgeon to determine if further surgery is feasible
- Options may depend on the state of the necrotic lung observed intra-operatively and what procedure(s) were previously performed. They may include:
- local packing and control of the bleeding source via thoracotomy
- lobectomy or pneumonectomy
- consideration of angioembolisation in selected cases
Notify the family
- Family must be notified that the patient has significantly deteriorated
- Explanation is best provided in a face-to-face meeting with senior clinicians and the family will need ongoing support
- Unless the haemorrhage can be corrected, the patient is likely to become unsupportable and the goal of care may need to shift from curative intent to palliation
References and Links
- Nickson CP. Massive transfusion protocol. Critical Care Compendium, Lifeinthefastlane.com [Accessed 22 November 2016] Available at URL: http://lifeinthefastlane.com/ccc/massive-transfusion-protocol/