Author: Jo Simpson
Reviewer: Chris Nickson
Everything ECMO 004
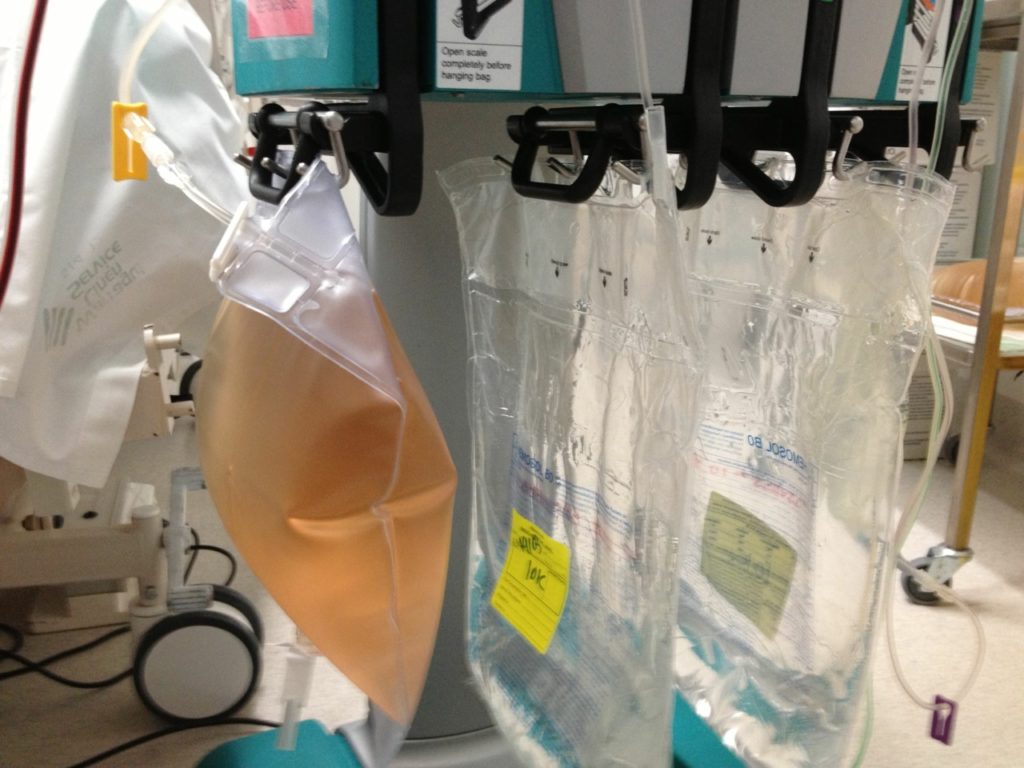
A 40-year-old man is receiving VA ECMO support following an out-of hospital cardiac arrest. He is also receiving continuous renal replacement therapy (CRRT) for an acute kidney injury. The nurse comes to tell you that the effluent bags of the CRRT have developed a reddish hue.
The nurse comes to tell you that the effluent bags of the CRRT have developed a reddish hue.
Q1. What laboratory test should you perform next?
Check a plasma free haemoglobin (PFHb).
This is the most sensitive test for haemolysis.
The laboratory test result is 1.2g/dL.
Q2. What does this mean and what are the possible causes?
The result suggests significant haemolysis complicating ECMO. The 2013 ELSO guidelines state that PFHb should be <0.1 g/dL under most conditions and that PFHb >0.5 g/dL should be investigated as to the cause.
Haemolysis affects about 1 in 5 ECMO patients (according to a meta-analysis by Zangrillo et al, 2013). Haemolysis does not occur during ECMO unless there is a problem in the circuit or the patient. Haemolysis in ECMO patients is associated with acute kidney injury and multi-organ dysfunction.
ECMO-related causes include:
- Access insufficiency (negative inlet pressures may reach -700 mHg resulting in cavitation and blood trauma; under normal conditions inlet pressures should be <-300 mmHg)
- Pump head thrombosis
- Oxygenator thrombosis
Haemolysis due to shear stress is less common with modern centrifugal pumps than it was with the older roller pumps previously used for ECMO.
Of course, numerous “non-ECMO-related” conditions can also cause haemolysis (see haemolytic anaemia in the LITFL CCC). In critically ill patients always consider these possible causes:
- Transfusion reactions
- Sepsis
- Medications triggering immune responses
- Extracorporeal circuits (e.g. haemofiltration at high flows)
Q3. What is your approach to investigating this further?
Investigate further using a structured approach, such as this based on the Alfred ICU ECMO guidelines:
Assess for intravascular haemolysis
- Clinical
- Dark/red urine or CRRT effluent (haemoglobinuria suggests severe haemolysis)
- Laboratory:
- Hyperkalaemia
- Raised LDH
- hyperbilirubinaemia
Assess circuit for malfunction:
- Noisy pump head (suggests pump head thrombosis)
- Visible access insufficiency (lines ‘kicking’)
- High transmembrane pressure gradient +/- decreased post-oxygenator PaO2 (suggests oxygenator thrombosis)
If there is evidence of circuit malfunction and high PFHb:
- Call ICU Consultant and investigate the underlying cause of malfunction, which may require a new circuit, a new oxygenator or re-cannulation
If the circuit is functioning and there are no clinical signs of haemolysis:
- Repeat sample
- PFHb can be artificially increased due to poor phlebotomy technique or blood sample handling
- Consider low level haemolysis
- Access insufficiency without kicking, which is more common with multi-stage cannulae (echocardiography may confirm suck down)
- Vessel cannulae impingement, due to:
- pericardial collection
- retroperitoneal haematoma
- excessive pump speed settings (RPM) with small diameter cannulae
Q4. How often should routine plasma free Hb (PFHb) sampling be performed and what is a normal operating level?
PFHb is routinely checked 6 hourly to screen for haemolysis in ECMO patients at the Alfred ICU.
The “normal” PFHb level is <0.1 g/dL
References and Links
- ELSO Guidelines for Cardiopulmonary Extracorporeal Life Support Extracorporeal Life Support Organization, Version 1.3 November 2013 Ann Arbor, MI, USA [accessed 23 November 2016] URL: http://www.elsonet.org
- Leverett LB, Hellums JD, Alfrey CP, Lynch EC. Red blood cell damage by shear stress. Biophysical journal. 12(3):257-73. 1972. [pubmed]
- Murphy DA, Hockings LE, Andrews RK. Extracorporeal membrane oxygenation-hemostatic complications. Transfusion medicine reviews. 29(2):90-101. 2015. [pubmed]
Thank you. Very educational.
Hi everything on ECMO!
Your posts are super informative and of great value to me and my colleagues
…
As to the thread “Why is the bag turning red?”
Please check the first block in an answer for Q2 and for Q4 … I suppose there are a bit misleading numbers for hemolysis FPHb:
0.5 g/dL and 0.1 g/dL – whereas they mention 0.05 g/dL and 0.01 g/dL in ELSO guide (literally – 10 mg/dl and 50 mg/dl)
Regards,
Evgeniy Khomenko, MD,
Saint-Petersburg Russia