Labs and Lytes 016
Author: Vui Kian Ho
Reviewers: Owen Roodenburg and Chris Nickson
A 58 year-old man is admitted to ICU for hypotension secondary to decompensated CCF. He has a BMI of 45 (weighs 125kg) and known to have a left ventricular ejection fraction of 20%, diabetes mellitus and hypertension with underlying renal impairment. Over the last 6 hours, his urine output has averaged 10ml/h, despite IV 80mg frusemide bolus and increasing inotropic support to maintain a MAP > 70 mmHg. He is also dyspneic with increasing bibasal crackles. His CVP is 19 mmHg.
Here are some relevant blood investigations (coagulation profile was unremarkable):
ABG
| pH | 7.18 |
| pCO2 | 31 mmHg |
| pO2 ( on NP 4L/min) | 72 mmHg |
| HCO3 | 14 mmol/L |
| BE | -9 mmol/L |
UEC and Hemoglobin
| K | 5.5 mmol/L |
| Na | 132 mmol/L |
| Cr | 352 umol/L |
| Urea | 29.4 mmol/L |
| Hb | 84 g/L |
Q1. Would you ‘dialyse’ this man? Why or why not?
Yes. It is reasonable to start renal replacement therapy for fluid overload unresponsive to diuretics.
Indications for renal replacement therapy include:
- Fluid overload unresponsive to diuretics
- Hyperkalaemia (e.g. K > 6.5 or rapidly rising, especially if refractory to medical therapy)
- Symptomatic uraemia (especially if Urea > 35 mmol/L)
- Uncompensated metabolic acidosis (pH <7.1)
- Overdose with a dialyzable toxin (e.g. Li, toxic alcohols, salicylates, theophylline, sodium valproate)
- Severe temperature derangements (e.g. >40C)
- Severe electrolyte derangements (e.g. Na <110 or >160 mmol/L)
Q2. You are tasked to insert a vascular catheter for continuous renal replacement therapy. Where would you insert the catheter and why?
At The Alfred ICU our order of preference is:
- 1st choice: Femoral vein
- 2nd choice: Internal Jugular vein
- Last choice: Subclavian vein
The main reason is increased circuit run time with femoral vascular catheters (see Crosswell et al, 2014).
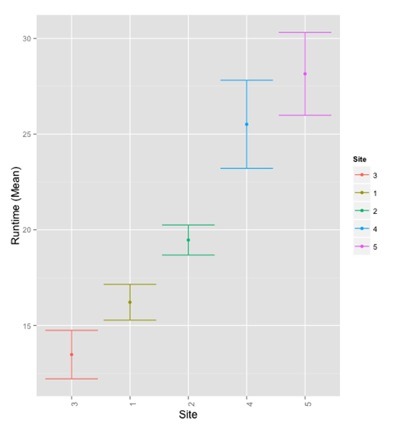
| Site | Mean run time (h) |
| Subclavian (3) | 14.38 |
| Internal jugular (1) | 17.09 |
| Femoral (2) | 20.20 |
| Tunnelled internal jugular (4) | 25.15 |
| ECMO circuit (5) | 28.97 |
There was significant difference between left or right sided insertion. Note that this data was with 14.5Fr tunnelled lines and 12.5Fr Vascular Catheters. Following this, the Alfred changed to 15.5Fr Vascular Catheters and will soon repeat the above analysis.
Premature circuit loss results in:
- Increased patient blood loss and blood transfusions
- Decreased effective RRT delivery
- Increased costs
As a point of interest, the KDIGO Clinical Practice Guidelines suggest the following order of preference: right internal jugular, femoral, left internal jugular and subclavian in the dominant arm as a last resort.
While subclavian vein catheters are more comfortable and have possibly the lowest infection rates, they pose greater complication risks such as deep vein thrombosis, pulmonary embolism, chronic limb oedema, and contraindication to formation of AV fistulae for long term dialysis in the setting of brachiocephalic vein thrombus and stenosis. They also provide relatively ineffective flows. As such they should be the site of last resort.
When to avoid the femoral veins
- Renal transplant patients – because of the risk of femoral vein thrombosis, which may seriously impair venous outflow from the transplant.
- When aiming for early mobilization, particularly in the case of patients with dialysis catheters.
- Massively obese – there may be a higher risk of CRBI and higher risk of access failure with femoral placement in some studies.
Q3. Hang on, what about the infection risk at different sites?
While the 2011 recommendations from “Healthcare Infection Control Practices Advisory Committee” of the Centers for Disease Control and Prevention advise to “Avoid using the femoral vein for central access in adult patients” (level 1A recommendation), this is not supported by a more recent meta-analysis by Marik et al (2012).
Marik et al’s meta-analysis found 2 RCTs and 8 cohort studies that met their inclusion criteria. There was no significant difference in the risk of CRBI between femoral and subclavian sites (i.e. no level 1A recommendation). The internal jugular site was associate with a significantly lower risk of CRBI compared to the femoral site, but this was explained by 2 studies with statistical outliers.
Q4. What size catheter would you use? What are the reasons for choosing this size?
About 14.5Fr is probably the optimal size.
Larger catheters are more prone to DVT formation. Smaller catheters will struggle to achieve blood flows of 200-300 ml/min, which is often required for adequate RRT and maximising the filter life.
Q5. How is catheter size measured? What does that mean in metric units?
French sizes.
The french size refers to the external circumference in millimetres. Hence the diameter of 1 Fr = 0.33 mm (by rounding down pi = 3).
Q6. You choose to insert the vascular catheter in the right femoral vein. Having inserted the vascular catheter a third of the way through over the guide-wire, you encounter great resistance and you notice the catheter starting to crumple.
What is happening? What can you do about this? What can you do to prevent this from happening next time?
Something is obstructing the passage of the vascath over the guide wire…
| Problem | Solution | |
| Patient problems | “Tough” skin | Ensure adequate dilation. Use scalpel to make a stab incision |
| Venous stenosis or extrinsic compression (e.g. tumours) | Change insertion site. May need a scan to confirm patent sites before proceeding | |
| Technique/ operator problems | In the wrong place – not in vein | Use ultrasound always (as recommended by most guidelines). Confirm guidewire placement. If unsure, start again. |
| Inadequate dilation | Ensure adequate dilation. Consider the use of the scalpel to make a stab incision | |
| Kinking of guidewire | Jiggle the guidewire during serial dilation and during insertion of dialysis catheter. If already kinked, change guidewire. | |
| Wrong angle of insertion making kinking more likely | “Long and low” approach. More common in femoral approach as depth to femoral vein is greater than internal jugular or subclavian. Exacerbated by greater adiposity. | |
| Equipment problems | Faulty designFaulty batch/ catheter | Change catheter. Change catheter model. Report the problem, speak to manufacturer. |
Q7. You decide to abandon the femoral approach and successfully inserted a vascular catheter in the right internal jugular. How far should you insert the vascular catheter? Why?
The tip of the catheter should be at the superior vena cava – right atrium junction or even in the right atrium for best flows.
Q8. What else should you do to increase the lifespan of the catheter you have just inserted?
Heparin lock, or the citrate equivalent (e.g. Sodium Citrate) if using a citrate-based RRT anticoagulation protocol (especially if known heparin hypersensitivity).
References and Links
- Crosswell A, Brain MJ, Roodenburg O. Vascular access site influences circuit life in continuous renal replacement therapy. Crit Care Resusc 2014; 16: 127-130 PMID: 24888283
- Foot CL, Fraser JF. So you need to start renal replacement therapy on your ICU patient? Curr Anaes & Crit Care 2005; 16: 321-329 [full text]
- Kidney Disease: Improving Global Outcomes (KDIGO) Acute Kidney Injury Work Group. KDIGO Clinical Practice Guideline for Acute Kidney Injury. Kidney inter., Suppl. 2012; 2: 1–138. [website]
- Marik PE et al. The risk of catheter-related bloodstream infection with femoral venous catheters as compared to subclavian and internal jugular venous catheters: A systematic review of the literature and meta-analysis. Critical Care Medicine 2012; 40:2479-2485. PMID: 22809915
When inserting at the IJ site, I prefer to puncture very low in the neck with an in plane approach to the anterolateral aspect of the IJV, rather than an out of plane approach to the anterior aspect. Then I rotate the catheter downwards toward the chest or supraclavicular region so I can place a proper dressing. I prefer to avoid a catheter that is oriented toward the ear because it is essentially impossible to maintain an intact dressing at this location.