Author: Aidan Burrell
Peer reviewers: Sacha Richardson, Arne Diehl, Chris Nickson
Everything ECMO 025
A 56-year-old man is being transported to your hospital following a witnessed ventricular fibrillation (VF) cardiac arrest. Bystander cardiopulmonary resuscitation (CPR) had been commenced with a no-flow time of approximately 5 mins. CPR is continuing, and the current low flow time is 45 mins. You are considering performing ECPR (extracorporeal cardiopulmonary resuscitation) on this patient.
Q1. What is the rationale for ECPR?
Even good CPR is not very effective, generating only approximately 25% of cardiac output.
ECPR can fully support the circulation, and therefore enables time for other treatments to work, such as percutaneous intervention (PCI) in ST-elevation myocardial infarction (STEMI), that can reverse the cause of the cardiac arrest.
Q2. The patient’s initial rhythm is VF. What impact does the initial rhythm have on overall outcomes for ECPR?
The initial rhythm has a large impact on overall outcomes.
Most ECPR studies only include patients with shockable (VF/VT) rhythm. PEA arrests are also included in several papers, and they have may have similar outcomes. However, this is a highly selected group of patients and don’t necessarily represent the outcomes of all PEA arrest patients. Asystole on initial rhythm is almost always fatal, and is commonly considered a strict contraindication for ECPR.
Q3. What do “no flow” time and “low flow” time mean?
No flow time is the time from arrest to the start of CPR
Low flow time is the time from the start of CPR to the commencement of ECMO.
Q4. What is the upper low flow time for initiating ECMO?
Most papers quote an upper limit of between 45-60 minutes, however, this is controversial.
In general, the sooner ECMO can be established, the better the outcome, and taking too long to establish ECMO is often the reason patients are excluded. However many case reports exist of patients with very prolonged cardiac arrests (>1.5hours) surviving neurologically intact.
Q5. What are the exclusion criteria for ECPR?
These are considered exclusion criteria for ECPR by the Alfred ICU ECPR Service:
- Age >65
- Unwitnessed
- Asystole
- No flow>10 mins
- Low flow time >60 mins
- Terminal illness
- Known severe neurological injury
In addition, certain physiological variables are associated with poorer outcomes.
- Lactate>18
- Ph<6.8
- ET CO2 <10
Despite the above list, no single criteria is discriminatory enough to predict a poor outcome by in itself. For example, having one of these bad markers may be offset with many other more favourable markers, and hence an overall good chance of survival. In practice, all variables need to be added together to get an overall picture and chance of success. Team-based decision making is very important.
Q6. Discuss how a more liberal vs a more restrictive selection criteria impacts survival in an ECPR program.
The selection criteria will impact on the total numbers and the survival rate. Designing a system with very strict criteria (eg only young, early, shockable) will likely result in a high survival rate. However this system will have low numbers of eligible patients, and almost certainly miss patients who could have benefited but were outside this criteria. On the other hand, more relaxed criteria will increase the numbers, but the survival rate will be lower. This will also use up scarce resources that could be used elsewhere.
Summary of important selection criteria factors:
| Factor | Impact on survival | Significance/Comment |
| Shockable Rhythm | +++ | Many use this as an inclusion criteria |
| Witnessed Arrest | ++ | Yes/No |
| Bystander CPR | + | Very important but not significant in some studies, especially if no flow time <10mins |
| Cardiac origin of CA | ++ | Extra-cardiac cause has survival in some groups |
| No flow time >10mins | — | 10mins commonest |
| Low flow time <60 mins | — | Variable in different systems |
| Older age>75 | — | Upper range between 60-75-year-old |
| Signs of life/moving during CPR | ++++ | Positive predictor |
| IHCA | ++ | OOHCA similar in some studies |
| Drug Overdose | ++ | Highly reversible cause of cardiac arrest |
| Hypothermia | + | Controversial, but may have a protective effect |
Q7. What is the evidence for ECPR compared to conventional CPR?
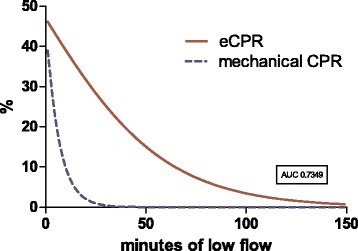
Survival in refractory CA over 30 minutes drops to approximately 0-10%2,3. With ECPR, survival with good neurological outcome range can increase to around 10-40%, even up to 30-60mins4,5. There are no randomized controlled trials comparing conventional to ECPR, but observational studies2,3,6,7 and systematic reviews4,5,8 of selective patients have found ECPR to be more effective than conventional CPR2,3,6,7,9.

Figure 2. Relation between CPR duration and the survival rate to discharge (from Chen et al, 2008)
References
- Wengenmayer T, Rombach S, Ramshorn F, et al. Influence of low-flow time on survival after extracorporeal cardiopulmonary resuscitation (eCPR). Crit Care. 2017;21(1):157. [pubmed]
- Soar J, Nolan JP, Böttiger BW, et al. European Resuscitation Council Guidelines for Resuscitation 2015: Section 3. Adult advanced life support. Resuscitation. 2015;95:100-47. [pubmed]
- Goto Y, Funada A, Goto Y. Relationship Between the Duration of Cardiopulmonary Resuscitation and Favorable Neurological Outcomes After Out-of-Hospital Cardiac Arrest: A Prospective, Nationwide, Population-Based Cohort Study. J Am Heart Assoc. 2016;5(3):e002819. [pubmed]
- Neumar RW, Shuster M, Callaway CW, et al. Part 1: Executive Summary: 2015 American Heart Association Guidelines Update for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2015;132(18 Suppl 2):S315-67. [pubmed]
- Yukawa T, Kashiura M, Sugiyama K, Tanabe T, Hamabe Y. Neurological outcomes and duration from cardiac arrest to the initiation of extracorporeal membrane oxygenation in patients with out-of-hospital cardiac arrest: a retrospective study. Scand J Trauma Resusc Emerg Med. 2017;25(1):95. [pubmed]
- Shin TG, Choi JH, Jo IJ, et al. Extracorporeal cardiopulmonary resuscitation in patients with inhospital cardiac arrest: A comparison with conventional cardiopulmonary resuscitation. Crit Care Med. 2011;39(1):1-7. [pubmed]
- Sakamoto T, Morimura N, Nagao K, et al. Extracorporeal cardiopulmonary resuscitation versus conventional cardiopulmonary resuscitation in adults with out-of-hospital cardiac arrest: a prospective observational study. Resuscitation. 2014;85(6):762-8. [pubmed]
- Ouweneel DM, Schotborgh JV, Limpens J, et al. Extracorporeal life support during cardiac arrest and cardiogenic shock: a systematic review and meta-analysis. Intensive Care Med. 2016;42(12):1922-1934. [pubmed]
- Chen YS, Lin JW, Yu HY, et al. Cardiopulmonary resuscitation with assisted extracorporeal life-support versus conventional cardiopulmonary resuscitation in adults with in-hospital cardiac arrest: an observational study and propensity analysis. Lancet. 2008;372(9638):554-61. [pubmed]
Excellent review of the State of the art. Congrats!
Thanks Ivan!
Chris
You have defined the following:
No flow time is the time from arrest to the start of CPR
Low flow time is the time from arrest to the commencement of ECMO.
Rather, the Low Flow Time should be defined as time from onset of CPR (incl bystander CPR) to the commencement of ECMO?
Thanks Sohil
You are correct and we have corrected the text.
The terminology can get very confusing!
Given that most goodECPR candidates are witnessed arrests, or have CPR started very soon after the arrest, the times tend to be similar – however, time from arrest to start of ECMO is better considered “total arrest time”, which is the sum of “no flow time” and “low flow time”.
Cheers
Chris