Labs and Lytes 005
Author: Nick Bingham
Reviewer: Chris Nickson
A 60 year-old man has been in ICU for 2 weeks, having presented with with respiratory failure requiring ECMO after an oesphageal rupture. Day 6 after starting piperacillin/tazobactam (tazocin) for a likely chest infection, he developed fevers. Blood cultures and a septic screen were sent. He developed acute kidney injury and renal replacement therapy was initiated.
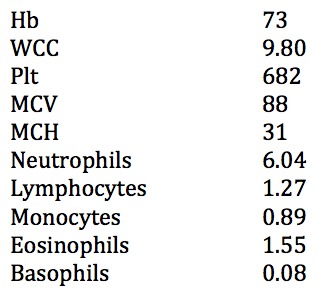
This is his full blood count:
Q1. What are the important findings on the full blood count?
The FBC findings are:
- normocytic anaemia
- thrombocytosis
- normal WBC, neutrophils and lymphocytes
- eosinophilia
Q2. What should you suspect as the cause of the fever?
The film above shows a peripheral eosinophilia. In association with fevers with no obvious infective source, in the setting of a recently started beta-lactam and renal impairment, this is likely a drug fever.
A drug fever is defined as: “a disorder characterized by fever coinciding with administration of the drug and disappearing after discontinuation”. Obviously it is important to exclude other causes of fever, sepsis being most common. The diagnosis of drug fever is often tricky to make.
Fever can be the sole manifestation of an adverse drug reaction (in 3-5% of ADRs). Median onset of fever after commencing the drug is 8 days (ranges from 24hrs to months). A peripheral eosinophilia occurs in only <20% of drug fevers. Up to 10% of ICU patients may experience a drug-induced fever.
Risk factors for drug fever include being elderly or being HIV positve (at increased risk of ADRs in general)
Drug rashes and deranged liver or renal function are common.
After stopping the trigger drug, drug fevers will typically decrease within <72 hours. Fevers associated with drug rashes, however, may last for days or weeks.
Q3. What would the presence of urinary eosinophils signify?
Urinary eosinophils are consistent with acute interstitial nephritis as the cause of renal impairment. Piperacillin/tazobactam is an important cause of this.
Check for urinary eosinophils if there is renal impairment and the patient is on a drug that cause acute interstitial nephritis. The positive predictive value is probably low in ICU patients, however.
Drugs that can cause interstitial nephritis include:
- Antimicrobials — penicillins, cephalosporins, sulfonamides; also: ciprofloxacin, isoniazid, tetracyclines, vancomycin, acyclovir
- NSAIDs
- Diuretics — frusemide, thiazides
- Antihypertensives — ACE inhibitors such as captopril, calcium channel blockers such as diltiazem and amlodipine
- Anti-epileptics — phenytoin, carbamazepine
- Ulcer prophylactics — omeprazole, ranitidine
- Others — allopurinol, azathioprine, quinine, PTU, mesalazine
Renal biopsy is the definitive diagnostic test, but this is not usually performed unless the cause is unclear, or if there is no improvement following discontinuation of the suspected offending agent.
References and Links
- Cunha BA. Clinical approach to fever in the neurosurgical intensive care unit: Focus on drug fever. Surg Neurol Int. 2013 May 6;4(Suppl 5):S318-22. doi: 10.4103/2152-7806.111432. Print 2013. PubMed PMID: 23878765; PubMed Central PMCID: PMC3717527.
- Kodner CM, Kudrimoti A. Diagnosis and management of acute interstitial nephritis. Am Fam Physician. 2003 Jun 15;67(12):2527-34. Review. PubMed PMID: 12825841. [Free Full Text]
- McDonald M and Sexton D. 2014. Drug fever. In: UpToDate. Weller F (Ed), UpToDate, Waltham, MA. (Accessed 15/04/2014)