Author: Dr Matthew Durie, Dr Vinodh Nanjayya
Peer reviewer: Dr Aidan Burrell
Ferguson N, et al. Impact of non-pharmaceutical interventions (NPIs) to reduce COVID19 mortality and healthcare demand. 16 Mar 2020; doi.org/10.25561/77482
Last week saw the release of Imperial College COVID-19 Response Team’s Impact of non-pharmaceutical interventions (NPIs) to reduce COVID-19 mortality and healthcare demand. Several countries, including the United Kingdom (UK), have changed their strategy from mitigation to suppression to control the COVID-19 pandemic based on this white paper.
Using a previously published influenza pandemic simulation model and using COVID-19 characteristics from both published literature and expert opinion, the paper discusses feasibility of suppression and mitigation strategies in UK and the United States of America (USA). Table 1 provides a general comparison between the two strategies.
The paper estimated the impact of five non-pharmaceutical interventions (NPI): home isolation of cases, home quarantine of contacts, social distancing of those over 70 yrs of age, social distancing of the whole population and closure of school and university – on meeting the surge capacities of ICU beds in UK and USA.
Table 1. Comparison of suppression and mitigation strategies for control of an epidemic
| Impact | Disease Suppression Strategy | Disease Mitigation Strategy |
| Reproduction number (R) | Aims to reduce R to <1, i.e., reverse the epidemic curve and reduce the number of cases to low levels to eradicate the human-human transmission over time. | Aims to reduce R but not to less than 1 i.e., slow the spread of the disease. This leads to flattening of the epidemic curve. This strategy does not reduce the total number of cases. |
| Population immunity (PI) | Does not allow PI to build up as the number of cases in the population is small. There is an increased risk of a resurgence of the disease after the relaxation of the disease control measures. Therefore, disease control measures need to be sustained for an extended period of time till an effective treatment or vaccine becomes available. | Allows population immunity to build up over a period of time leading to eventual decline of the infectious disease. |
| Social and economic costs | Enormous | Less compared to suppression strategy. |
Impact of Unmitigated Epidemic:
Based on the simulation, assuming that seeding of COVID-19 occurred in January 2020 in UK/USA, without any mitigation efforts the peak mortality is reached at three months, and the ICU bed capacity will be exceeded by the second week of April 2020. The ICU bed demand will be 30 times greater than the maximum beds available in both UK and USA. The projected number of deaths is 50,000 in UK and 2.2 million in USA.
Impact of Mitigation Strategy with NPI (Figure 1)
Under the mitigation strategy, the combination of case isolation, home quarantine and social distancing of high-risk people for three months around the peak of the epidemic would reduce the peak ICU demand by two thirds and halve the number of deaths to 250,000 in UK and 1.1-1.2 million in USA. However the peak demand would still be eight times higher than the maximum available ICU beds in both UK and USA.
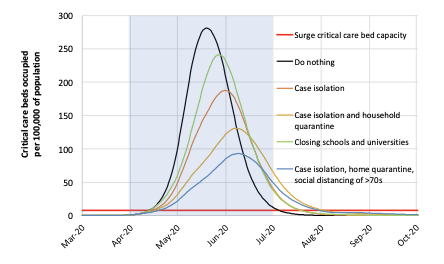
Figure 1. Mitigation strategies and impact on critical care bed occupation in the United Kingdom. Under every combination of NPI, critical care bed surge capacity is exceeded. The intervention is on for three months and social distancing of >70s is for four months. (Source: doi.org/10.25561/77482)
Impact of Suppression Strategy with NPI (Figure 2)
A suppression strategy using school and university closure, case isolation and general social distancing would reduce the peak critical care demand in 3 weeks to a level below the UK surge capacity of ICU beds. However, the timing of this intervention is crucial and for UK, this is before the number of new COVID-19 cases in ICU exceeds 200 per week. Also, these interventions need to be maintained for five months in the model to achieve disease suppression. Disease resurgence can occur due to the high proportion of susceptible people after the relaxation of NPI. China has achieved disease suppression using lockdown measures along with the NPI mentioned in the paper and it needs to carefully monitor for resurgence while relaxing the NPI.
The main challenge for this strategy is that the NPI measures are highly disruptive to social life and economy, and limited population uptake will not achieve suppression.

Figure 2. Suppression strategies and impact on critical care bed occupation in the United Kingdom. Panel B is zoomed in on the lower levels of graph in panel A. The blue shaded area represents the period during which the NPI is in place. The NPI combination of closure of school and university, case isolation and general social distancing is the only strategy that does not exceed the critical care bed surge capacity in UK when the interventions are in place. A resurgence of disease is predicted if NPI is relaxed after September 2020. (Source: doi.org/10.25561/77482)
Discussion
This paper provides a fascinating and timely analysis of the impact of various non pharmacological interventions on the scale, shape, and long term impact of COVID 19 on the UK and US populations.
The main drawback is that the modelling used in the study is dependent on many assumptions which may prove to be incorrect:
- The COVID-19 disease is new, and therefore much of the epidemiology remains uncertain
- Assumptions in the model, such as those obtained through early experience papers with small numbers of patients, or those provided by expert opinion, may prove to be wrong
- Data based from China may not be generalisable to other countries with different health care systems, social policy, and preparedness.
The authors did not include the impact of school and university closure on the availability of health care workers in ICU.
The authors also describe an adaptive suppression strategy where the NPI measures of social distancing and closure of schools and universities can be turned “off” and “on” based on the incidence of COVID-19 cases in ICU. By doing this, one-third of the time during the epidemic the NPI measures of social distancing and school/University closure can be relaxed.
Overall, this is a key paper in the control of COVID-19 pandemic using NPI. The paper provides a clear picture of the impact of various NPI on ICU surge capacity for COVID-19 cases. The paper concludes that suppression strategy which includes school and university closure, case isolation and general social distancing is the best strategy to control COVID-19 epidemic in UK and USA. While UK centric, the concepts appear applicable to other similar systems, including Australia and New Zealand.
Further reading:
- Ferguson N, Laydon D, Nedjati-Gilani G et al. Impact of non-pharmaceutical interventions (NPIs) to reduce COVID-19 mortality and healthcare demand. Imperial College COVID-19 Response Team. 2020 Mar 16. https://doi.org/10.25561/77482
- Mahase E, Covid-19: UK starts social distancing after new model points to 260 000 potential deaths. BMJ 2020;368:m1089, 2020 Mar 17. https://doi.org/10.1136/bmj.m1089
- Zhao S, Lin Q, Ran J et al. Preliminary estimation of the basic reproduction number of novel coronavirus (2019-nCoV) in China, from 2019 to 2020: A data-driven analysis in the early phase of the outbreak. Int J Infect Dis. 2020 Jan 27: 214-217. https://doi.org/10.1016/j.ijid.2020.01.050