Author: Jake Barlow
Reviewer: Chris Nickson
Journal Club 018
Murphy GJ, Pike K, Rogers CA, Wordsworth S, Stokes EA, Angelini GD, Reeves BC; TITRe2 Investigators. Liberal or restrictive transfusion after cardiac surgery. N Engl J Med. 2015 Mar 12;372(11):997-1008. doi: 10.1056/NEJMoa1403612. PubMed PMID: 25760354.
THE QUESTION
- Does a restrictive threshold for haemoglobin level in red-cell transfusions, as compared with a liberal threshold, reduces postoperative morbidity and healthcare costs after cardiac surgery?
STUDY DESIGN
TYPE OF STUDY
- A multicentre parallel-group randomised controlled trial
POPULATION
- 17 centers in the UK
- non-emergency cardiac surgery patients
- Patients were assessed for eligibility prior to their operation, and only randomised if their haemoglobin dropped below 90g/L in the post-operative period
- 11,483 were assessed for the study. Of these, 696 were not eligible, and 2359 (21%) were not assessed for other reasons.
- Of the 8428 patients who were assessable for eligibility, 281 were ineligible, 1863 (22%) were not approached, and 2719 did not consent. This left 3565 patients who were consented for participation, though 94 were later excluded, leaving 3471 to be considered for randomisation.
- 1464 patients were not randomised, 1288 because they did not breach the haemoglobin threshold and 176 (12%) patients because they were missed.
- In total, 2007 patients (17% of total patients assessed) were randomised by an off-site online system with concealed allocation, and minimised against centre and type of surgery. Notably, 4398 potentially-enrollable patients (38.3% of total patients assessed) were missed at some point prior to randomisation.
- Exclusions
- age <16 years-old
- religious beliefs precluded transfusion
- coexistent disorders of coagulation, sepsis, or critical limb ischaemia
- enrolled in another research trial
- otherwise unable to give informed consent
INTERVENTIONS/ COMPARISONS
Patients with a postoperative hemoglobin level of less than 9 g per deciliter were randomly assigned to:
- a restrictive transfusion threshold (hemoglobin level <7.5 g per deciliter) or
- a liberal transfusion threshold (hemoglobin level <9 g per deciliter)
OUTCOMES
| Comparison of characteristics of Treatment Groups with Alfred ICU Cardiothoracic Patients | |||
| Characteristic | Restrictive-threshold (n=1000) | Liberal-threshold (n=1003) | Alfred ICU 2010-2014 (n=2370) |
| Age (mean) | 69.9 | 70.8 | 66.6 |
| Operation N (%) | |||
| CABGs only | 408 (40.8) | 408 (40.7) | 1283 (58.8) |
| Valve only | 307 (30.7) | 304 (30.3) | 543 (24.9) |
| CABGs & valve | 195 (19.5) | 203 (20.2) | 302 (13.8) |
| Aortic surgery* | 54 (5.4) | 62 (6.2) | 54 (2.5) |
| NYHA III-IV N (%) | 297 (29.7) | 276 (27.4) | 247 (10) |
| Mortality** | 26 (2.6) | 19 (1.9) | 33 (1.5) |
| *Classifications of aortic surgery differ between TITRe2 and ANZICs ** TITRe2 mortality for 90 day survival, Alfred ICU survival to hospital discharge |
|||
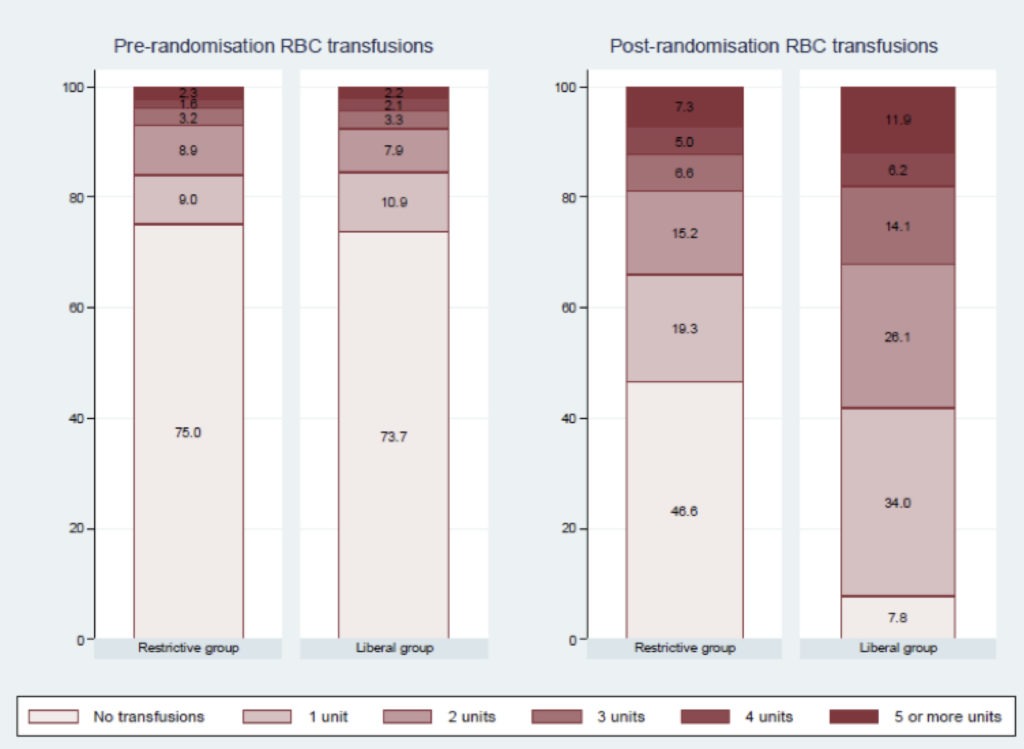
- After randomisation, the transfusion rate was 53.4% in the restrictive-threshold group vs. 92.2% in the liberal-threshold group. Groups differed significantly on the number of units transfused
Primary outcome
- Composite primary outcome of infective (sepsis, wound infection) and ischaemic (CVA, MI, gut ischaemia, AKI) events
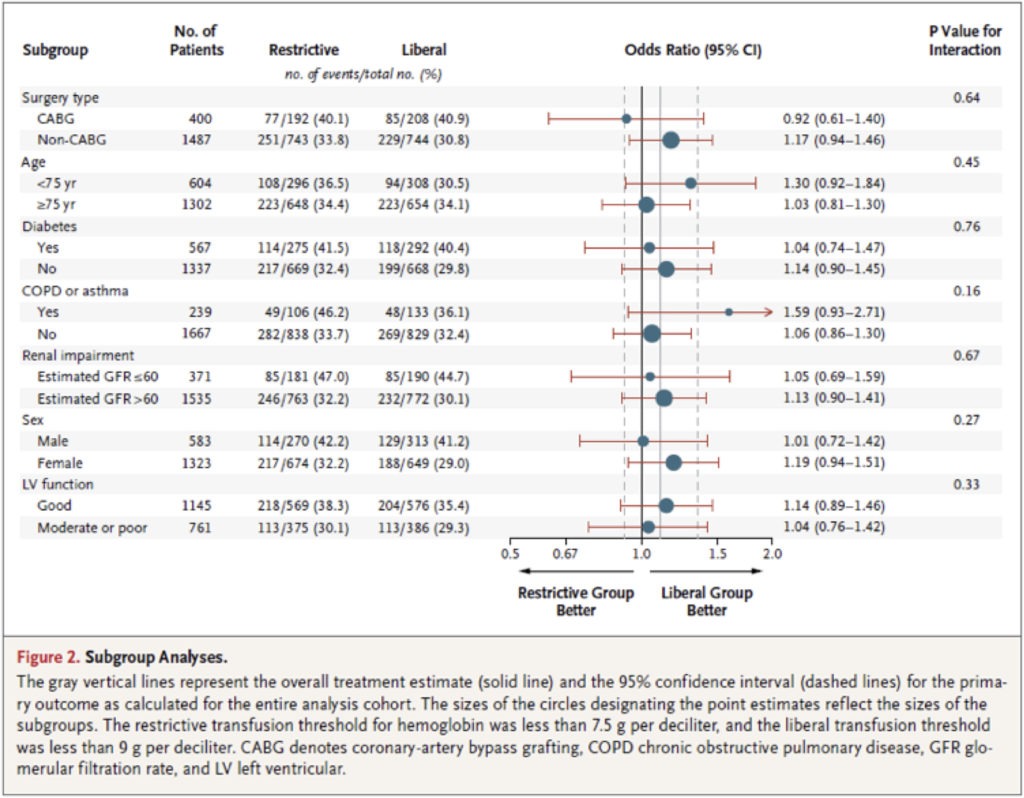
- The primary outcome occurred in 35.1% of the restrictive group and 33.0% of the liberal group and showed no significant difference (OR 1.11, 95% CI 0.91 to 1.34, p=0.30). Subgroup analyses were performed for a number of different patient characteristics, but none of these reached significance.
Secondary outcomes
- Pre-specific secondary outcomes included ischaemic events, infective events, transfusion requirement, duration of ICU, HDU, and hospital admission, and all-cause mortality.
- Mortality was significant with an increased number of deaths in the restrictive-threshold compared to the liberal-threshold group (4.2% vs 2.6%, HR 1.64, 95% CI 1.00 to 2.67, p=0.045).
CRITICISMS AND COMMENTARY
Criticisms
- Assessors were blinded to patient assignment though treating clinicians were not, which understandable given that doing so is impracticable. Patients were intended to be blinded to allocation, and were surveyed to determine whether this was successful though these results were not published by the authors
- Results were missing for 25 (1.2%) of patients, and severe nonadherence (such that it changed the classification with respect to receipt of transfusion) occurred in 97 patients (9.7%) in the restrictive group and 62 (6.2%) in the liberal-threshold group
- The primary outcome was a composite outcome, presumably used to increase the chance of detecting a significant difference between groups given that adverse outcomes are relatively rare. It is questionable whether the component outcomes are equivalent to one another.
- The secondary outcome suggesting a mortality difference should be treated with caution. The mean Hb difference between groups was a modest 10g/L, which seems disproportionate to the relatively large change in the hazard rate. The authors suggest that patients with cardiovascular disease may be a specific high-risk group that would benefit from a more liberal transfusion threshold, and that this result is worthy of further study. However, it may simply be a statistical artefact.
- Measurement was performed through serial blood tests. Notably, the creatinine threshold for defining acute kidney injury (AKI) was different in different centres, which resulted in a failure to identify some events of AKI.
Commentary
- Ethics approval was received from a NHS research ethics committee
- The study protocol was thoroughly designed, and the statistical plan was pre-published.
- Sample size calculations were performed and the study was powered for an effect size of 6%. Estimates of the incidence of the primary outcome were based on the authors previous work, and in fact underestimated the rate of occurrence in this study
- Prior to this study practice was highly variable, with different centres transfusing as few as 5% or as any as 90% of their patients undergoing CABGs (Spertus, 2015)
- Patient groups were comparable at baseline, though in general had more severe cardiac disease than patients seen at The Alfred ICU
- The primary outcome results differ from previous observational trials, but align with those of the Cochrane review.
FINAL WORDS
- A liberal transfusion threshold after non-emergency cardiac surgery is not indicated in unselected patients.
REFERENCES AND LINKS
- Murphy GJ, Pike K, Rogers CA, Wordsworth S, Stokes EA, Angelini GD, Reeves BC; TITRe2 Investigators. Liberal or restrictive transfusion after cardiac surgery. N Engl J Med. 2015 Mar 12;372(11):997-1008. doi: 10.1056/NEJMoa1403612. [pubmed]
- Spertus J. “TITRe”ing the approach to transfusions after cardiac surgery. N Engl J Med. 2015;372:(11)1069-70. [pubmed]